Given the recent Omicron surge, it is time to reassess the workloads of infection preventionists (IPs) to make sure they can focus on critical patient safety and infection surveillance, rather than administrative tasks.
So says the Association for Professionals in Infection Control and Epidemiology (APIC) in a recent article in Healthcare Hygiene Magazine.
“IPs are the only healthcare professionals with specialized expertise in spotting clusters of infections and integrating evidence-based strategies to limit their spread,” APIC President Linda Dickey says in the article.
APIC has created a free, downloadable tool called the IPC Acuity Scale that sorts infection prevention and control tasks into categories considered high priority and those that can be handled by non-IP staff, or even set aside given the pandemic.
“If our nation’s IPs are bogged down with data entry and other administrative work, they are less able to protect patients and staff from COVID transmission or the spread of drug-resistant organisms,” Dickey says.
Protecting healthcare workers from contracting the novel coronavirus and other infections is important in every clinical area of the hospital.
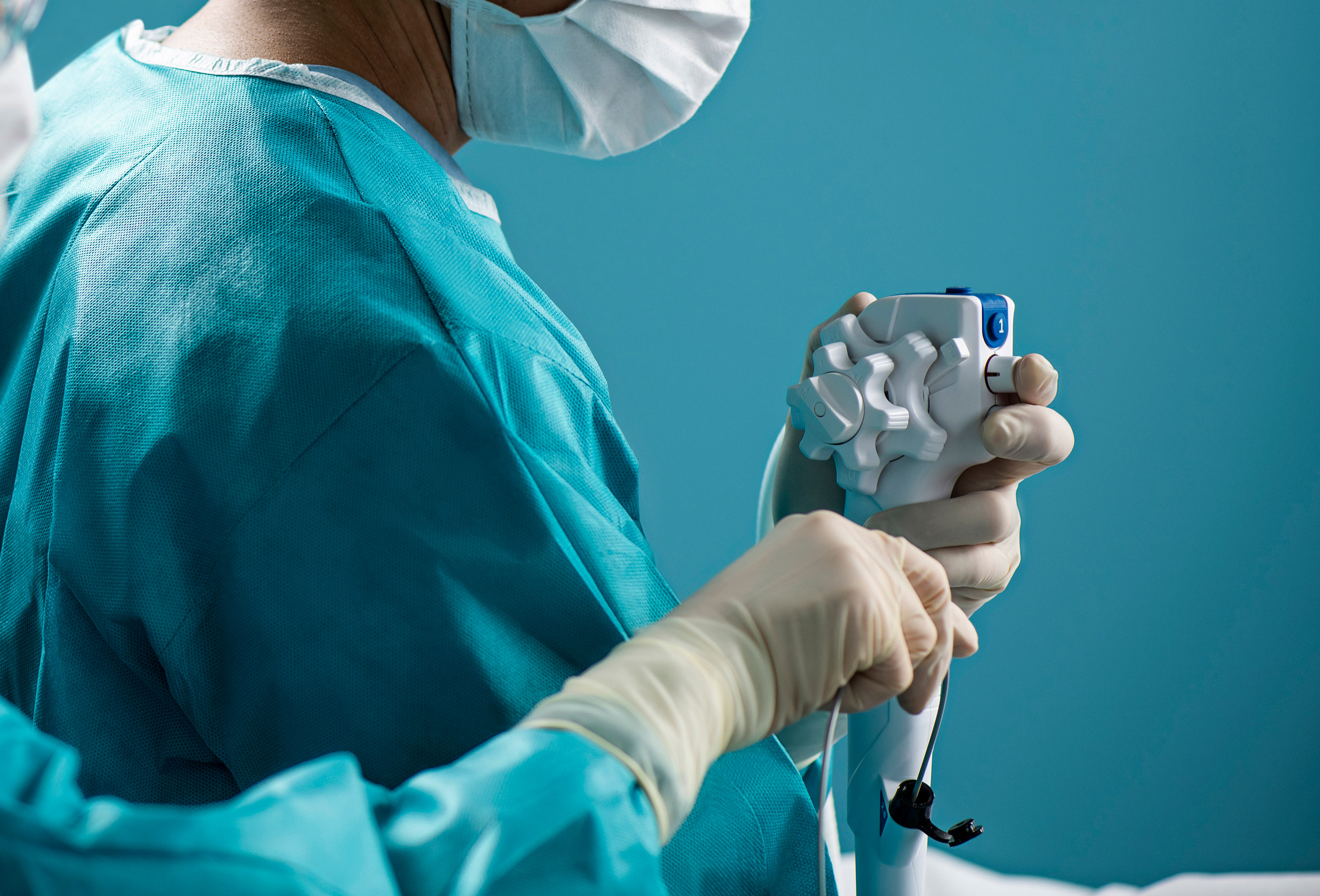
Endoscopy suites, along with ICUs and bedsides around the world are among the places where single-use endoscopes can help IPs do their jobs by keeping patients and staff safe from rare cases of cross-contamination from inadequately cleaned reusable scopes.
The safety net that single-use bronchoscopes can provide in ICUs has never been more evident than during peaks in the COVID-19 pandemic as patients crowded into hospitals. With heightened infection awareness, some patients have even started to request single-use endoscopes, physicians say.
The U.S. Food and Drug Administration (FDA) has recommended considering the use of single-use bronchoscopes when there is increased risk of spreading infection or when there is no support for immediate reprocessing — regulatory guidance that is helping drive conversion to single-use endoscopy.
Routinely, IPs set an organization's standards for the hygiene and personal protective equipment (PPE) of patients, staying vigilant for infection. The global pandemic, however, has added new layers to their job. IPs are now navigating challenging PPE supply chains, ensuring that hospitals have adequate surge capacity plans, and keeping ever-shifting infection guidance is up to date.
The current heavy workload for IPs comes at a time when they already are in short supply.
A report in Infection Control Today estimates that 40 percent of infection preventionists are due to retire in the next 10 years.
Not only has COVID-19 escalated the need for IPs, it also has expanded their potential workplaces to include airlines, schools, cruise ships, workplaces and elsewhere.