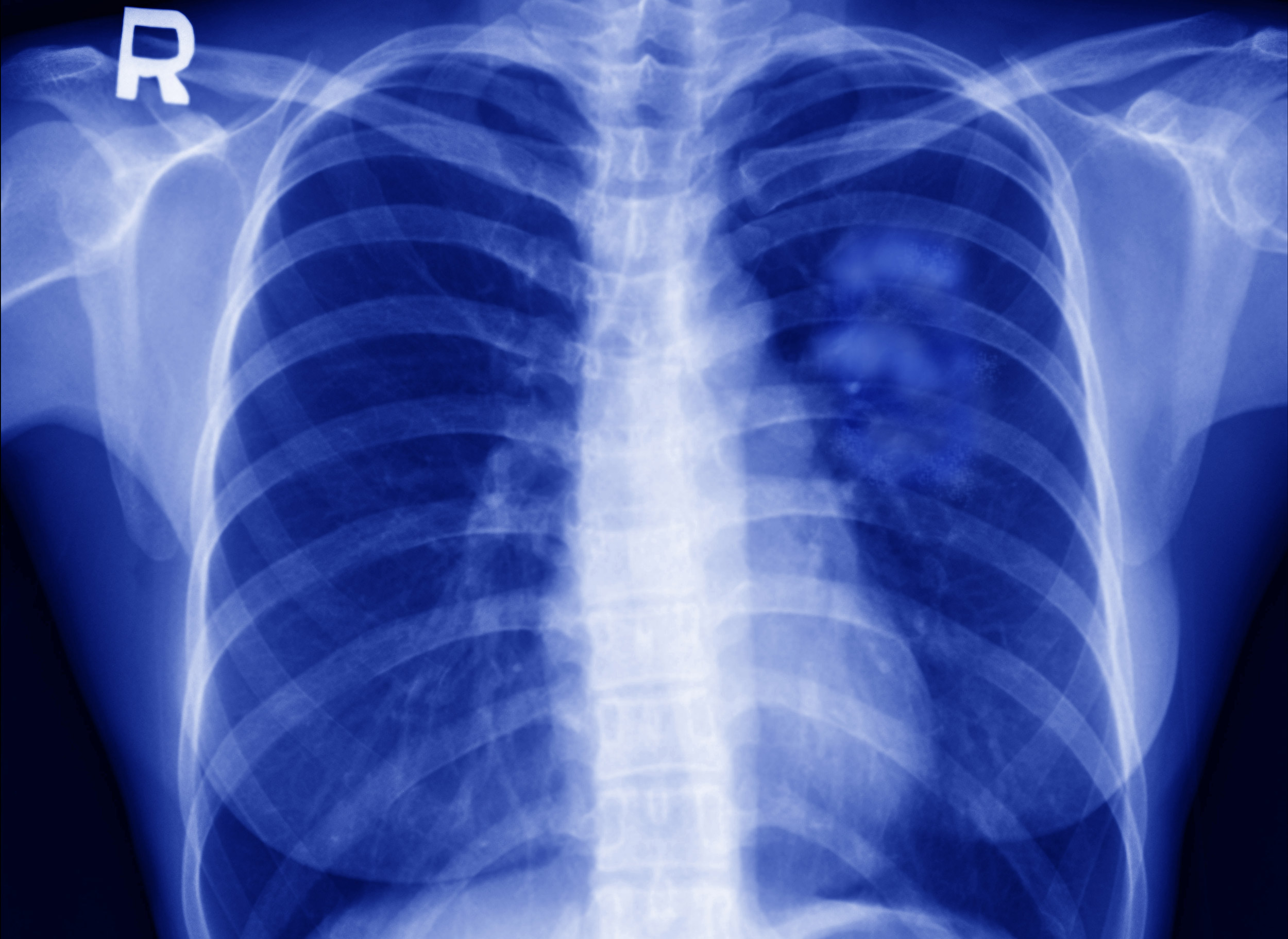
Lung cancer, the second-leading cause of death among women worldwide, represents a global health crisis for women.
But despite having a higher risk for the disease with adjustments for age, stage, and histologic subgroups, women actually experience better outcomes following treatment for the disease than men. That's according to a Swedish study by Drs. Erik Sachs, Urik Sartipy and others, affiliated with Karolinska University Hospital in Stockholm.
That research, a nationwide population-based observational cohort study of 6,356 patients, found a survival advantage in women compared with men following lung cancer surgery. The study's authors reported the advantage for women held independent of age, socioeconomic status, common comorbidities, physical performance, type and extent of surgery, tumor characteristics, and stage of disease.
Women have a better survival rate than men that cannot be explained by smoking habits or life expectency, the researchers added.
In the study, most of the men and women who were diagnosed with lung cancer had a current or previous history of smoking. But the subset of patients that didn’t have a history of smoking, were more frequently women, 22.2 percent compared with 14.3 percent men.
Tobacco smoking is one of the most important risk factors of disease and mortality, the study notes. In that Swedish study, women more often were never smokers, whereas men were more likely to be former smokers.
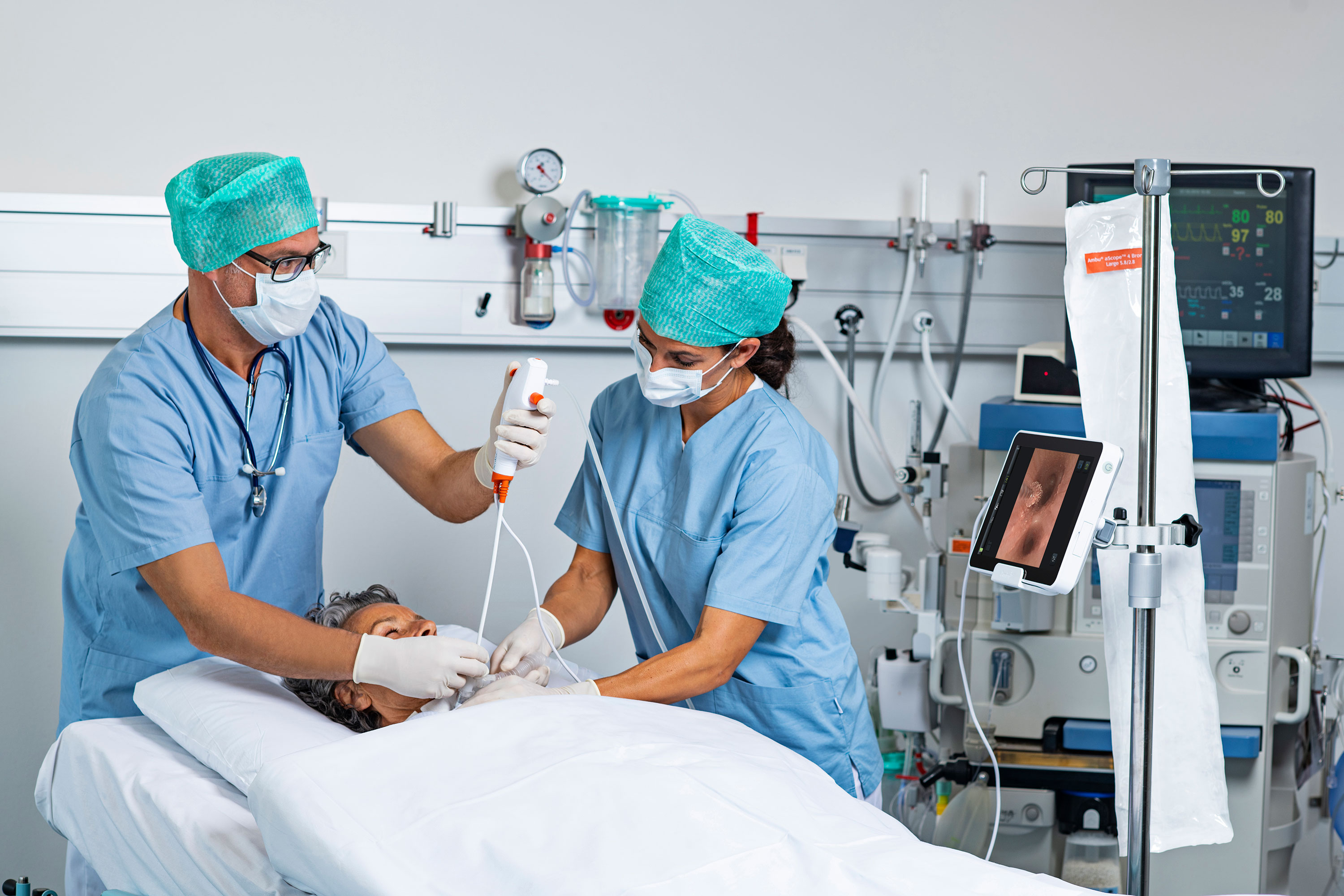
Bronchoscopy is typically used in the diagnosis, endoscopic study and treatment of the tracheobronchial tree and airways. Bronchoscopes help in detecting tumors, COPD, lung cancer, bronchitis, and other lung infections.
A rise in the number of lung cancer cases across the globe is expected to boost demand for single-use bronchoscopes, according to data from BioSpace. Aging baby boomers in teh U.S. contribute to a rise in people living with such chronic respiratory health issues as COPD. Single-use bronchoscopes require no reprocessing or repairs and eliminate the risk of cross-contamination, which is beneficial for immunocompromised cancer patients.
In a recent CHEST editorial in response to the Swedish study, Drs. Christina R. MacRosty and M. Patricia Rivera, both affiliated with the Division of Pulmonary Diseases and Critical Care Medicine at University of North Carolina, Chapel Hill, say more research is needed to understand this discrepancy between the outcomes for women and men.
They write the lack of research on sex-based differences in lung cancer limits understanding of reasons for both the higher risk of lung cancer and the improved survival rates among women. A lot remains unknown, the authors add.
“The double-edged sword of female sex and lung cancer necessitates that future studies aim to better understand factors (environmental, genetic, hormonal) in addition to smoking intensity and duration that may affect risk," they write.
The American Cancer Society (ACS) identifies lung cancer as the leading cause of cancer deaths in U.S.
For the most common form of lung cancer (non-small cell), the five-year relative survival rate for patients diagnosed at an early localized stage, is 63 percent. That's compared with a 7 percent relative survival rate for patients diagnosed at a later stage.
Researchers from the American Cancer Society and the National Cancer Institute report that lung cancer rates in young women are higher than those of young men, defined as people born since 1965. They describe those findings as “surprising,” since lung cancer rates in men have historically been higher. Also surprising is that differences in smoking patterns do not fully account for the change, the ACS says.
The researchers explore possible explanations in a study published in The New England Journal of Medicine. One is that women may be more susceptible than men to the health hazards of lung cancer, and women may be more likely than men to develop lung cancer even after they quit smoking.