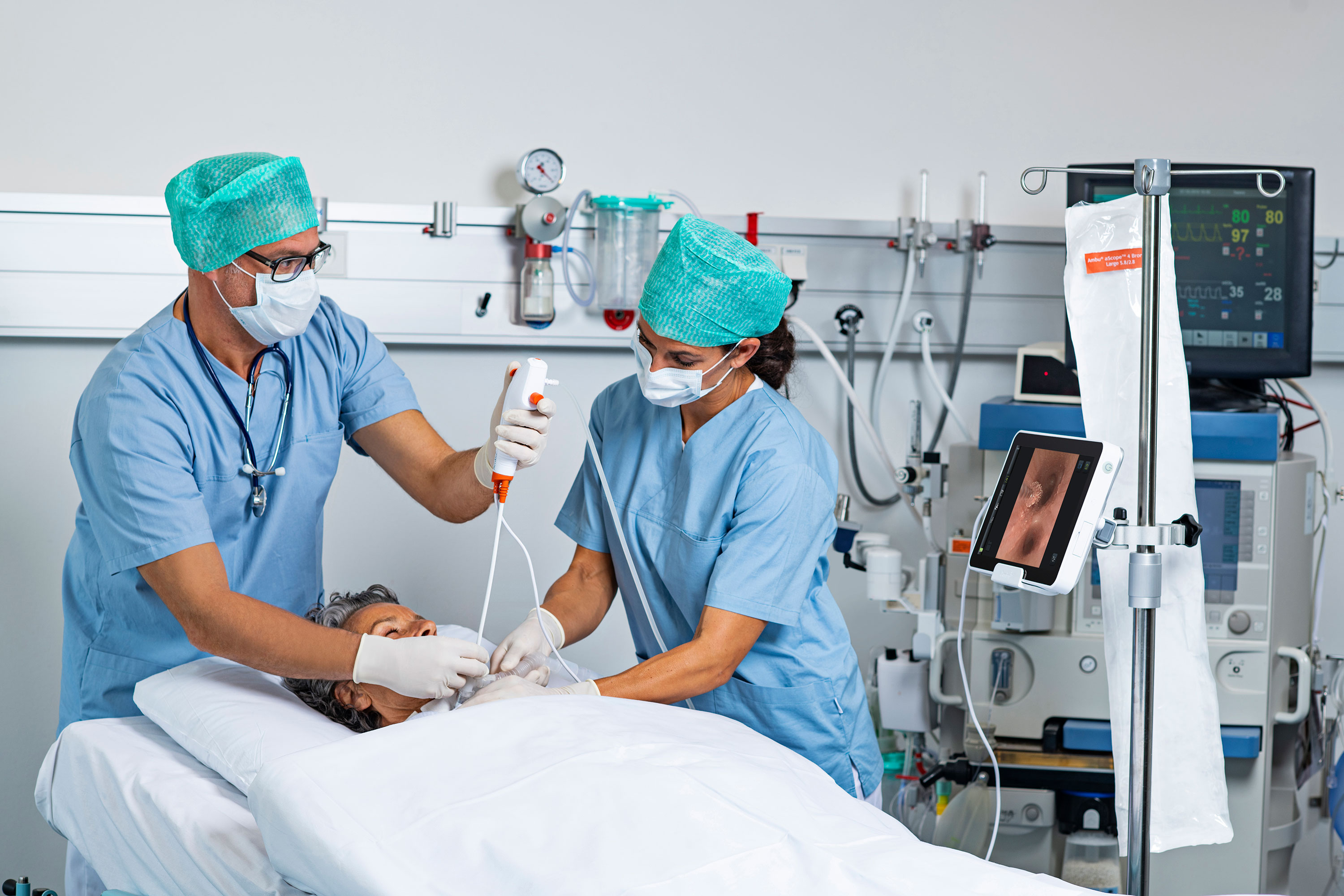
Magnification and borescopes found damage and residue or debris in all of the fully reprocessed endoscopes recently tested in a new study.
That study, by Cori L. Ofstead and others, which covered a two-month period in an endoscopy department just starting to use inspection tools, was published in the American Journal of Infection Control.
The research examined a variety of reusable endoscopes, including bronchoscopes, gastroscopes, duodenoscopes, and colonoscopes ranging in age from two years to 18 years.
Ofstead, president and CEO of Ofstead & Associates, has done extensive research on endoscope contamination, splash contamination during cleaning, and the value of PPE in protecting reprocessing staffers.
In this study, visible damage and residue or debris was found in 100 percent of the 25 endoscopes during two separate assessments, according to the research. Of those, 76 percent required repair.
“It is clear that visual inspection with lighted magnification is a necessary ‘safety timeout’ to protect patients from injuries and infections due to damaged or contaminated endoscopes,” the authors write. “Infection preventionists have a critical role to play in supporting processing personnel now that standards, guidelines, and IFU align with strong recommendations for enhanced visual inspection of every endoscope, every time.”
Adhesive band disintegration was found on 80 percent of the endoscopes tested — a problem because those damaged surfaces can harbor soil and bioburden. Yellow soil was found in adhesive gaps, and those sharp edges could injure patients and staff handling the endoscopes, the authors write.
"Scratches and shredding observed in channels of almost every endoscope, including those that were recently repaired or refurbished, echo previous findings by others who found that channels sustained damage within a few months of use and accumulated visible defects over time,” according to the authors.
Single-use endoscopes like those offered by Ambu are sterile straight from the pack and eliminate any need for reprocessing, repairs or borescope tests. They are simply used once and discarded, so each patient gets a brand new scope.
The new ANSI/AAMI ST91 standards, and new guidelines from AORN, recommend that personnel reprocessing reusable endoscopes be trained on use of borescopes. Ofstead and her co-authors, however, write that endoscope manufacturers have not yet provided guidance on how to conduct the examinations or how to decide whether results are normal or show a need for repair, further cleaning or other additional action.
Endoscopy personnel mastered the visual inspection tools after a few hours of training and support from the research team, the authors write.
A key change in the new guidance is that flexible endoscopes are now classified as “high-risk,” necessitating high-level disinfection to rid scopes of contaminants that could harm patients.
Given these recommendations, infection preventionists should take the lead to ensure that staff has adequate time, equipment and support to conduct inspections and address findings, according to the study.
Increasingly, there is a call for infection preventionists to play a larger role in providing perspective and oversight in endoscope reprocessing.