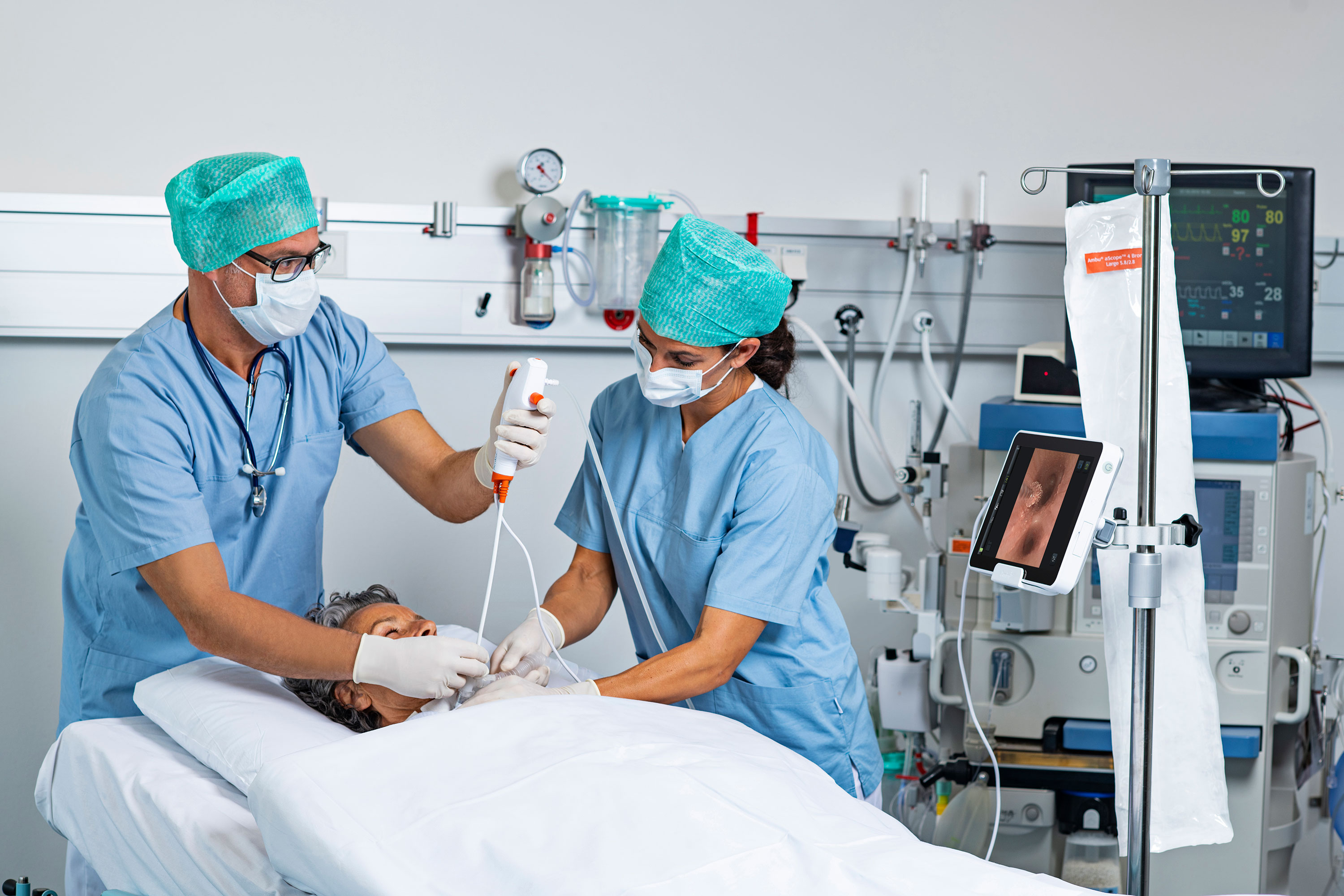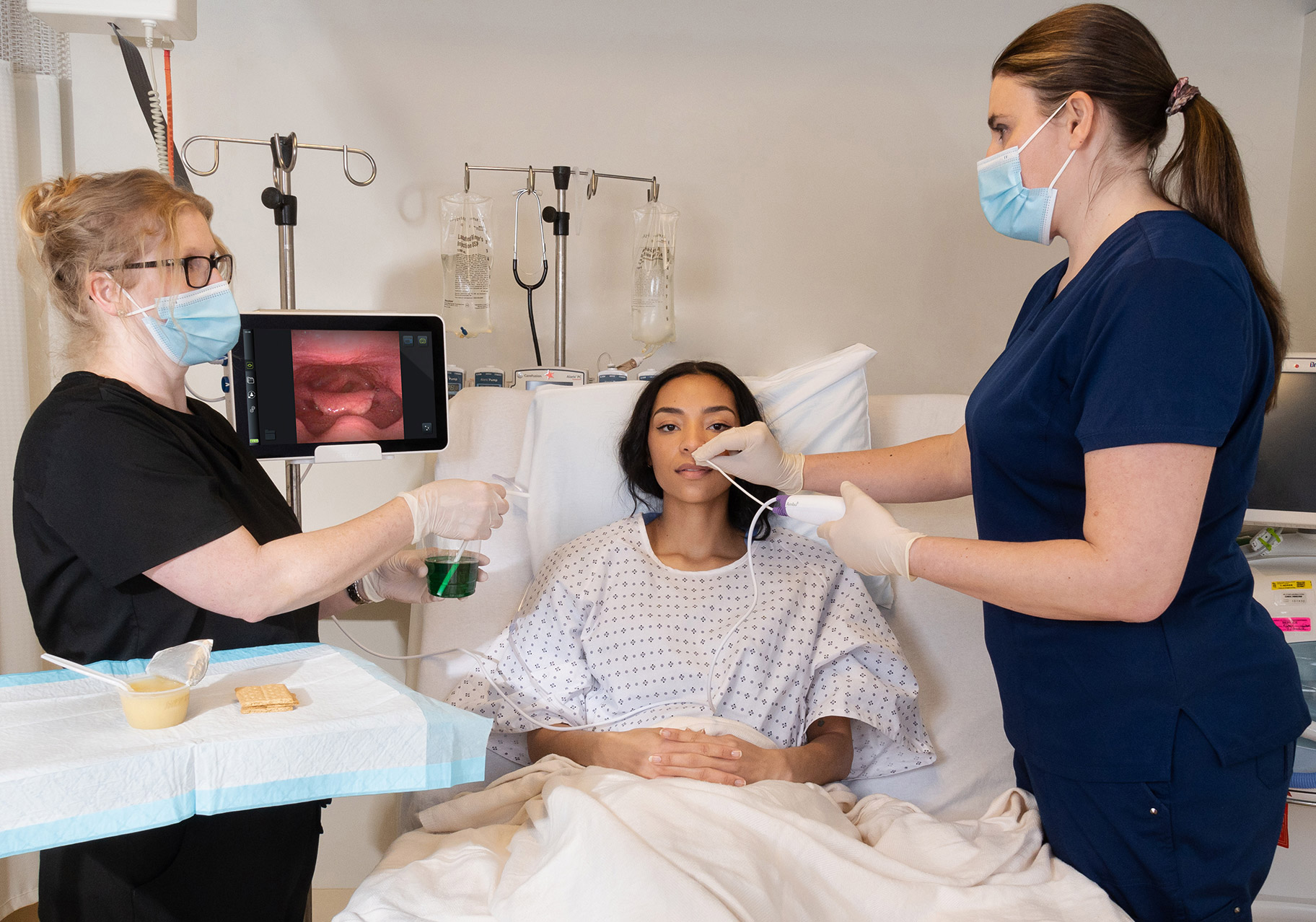
Traveling throughout North America to conduct trainings, Dr. Eric Blicker has encountered some reusable endoscopes that require a large tower system to operate. Although the image quality can be great, maneuvering a bigger system in some healthcare settings can be challenging.
For Blicker, who has 22 years of experience performing flexible endoscopic evaluation of swallowing (FEES) exams, it’s a stark reminder of the advantages of single-use devices to save time, energy and money — all in a small footprint with easy portability.
“The ability to just have a scope on the shelf definitely increases productivity,” says Blicker. “We’re not waiting. We’re going, going, going. We are having a positive impact on patient care “
 Blicker, (CCC-SLP.D) is president of Community Care Partners Inc. in Naples, Florida, which provides consulting services for continuing education as well as dysphagia evaluation and treatment. An outspoken advocate for single-use devices, he has worked and consulted in numerous healthcare settings over 24 years.
Blicker, (CCC-SLP.D) is president of Community Care Partners Inc. in Naples, Florida, which provides consulting services for continuing education as well as dysphagia evaluation and treatment. An outspoken advocate for single-use devices, he has worked and consulted in numerous healthcare settings over 24 years.
His clinical experience includes working in long-term acute care, inpatient acute care, outpatient hospitals, skilled nursing facilities, outpatient otolaryngology, and outpatient pulmonology settings.
He often works and teaches using single-use rhinolaryngoscopes paired with a monitor — a system designed for easy visual exams of patients suffering from dysphagia, post-extubation challenges or other laryngeal issues. Single-use devices eliminate the challenges of endoscope availability, reprocessing and complex towers.
In this Q&A, Blicker discusses the impact that single-use endoscopes have had on his clinical practice, and he contrasts single-use with reusable scopes in terms of both performance and cost factors.
SUE: How has using a single-use scope changed your clinical practice?
Blicker: It has changed my clinical practice by improving productivity without compromising quality. The easy access to equipment and time saved without the need for high-level disinfection are invaluable. The lightweight scope is great to avoid fatigue during the exam. It’s been something that’s changed my entire approach to medical care.
SUE: What is a typical day like for you and in what ways do workflow hurdles impact patient care?
Blicker: Workflow includes different settings and across these different settings come different facility expectations. Infection control, evolving COVID-19 guidelines, staffing, and productivity are some of the hurdles that clinicians and I encounter.
SUE: How important is immediate access to scopes, and why? How does it help on nights and weekends?
Blicker: Immediate access is critical as length of stay is an important aspect of care, as are any delays in patient care. Many traditional endoscope systems are kept in endoscopy settings, not near patient care areas. To have access without delay expedites the treatment process. In my experience of 24 years in hospitals, it is not uncommon for patients to wait for transportation to modified barium swallow (MBS) testing. With single-use equipment, this is completely avoided because of immediate access, which facilitates scheduling. With the single-use scope, we are not reliant on radiologists, radiology scheduling for MBS or endoscopy schedules to clean scopes. These are often departments with less staffing on weekends and later in the day.
SUE: Has there been a shift from MBS testing to FEES exams and if so, why? Is demand growing for the procedure and clinicians who perform it?
Blicker: When there is a lack of objective assessment like FEES available, the speech language pathologist may have to base their dysphagia management on subjective information along with observed signs and symptoms of dysphagia. This can result in both overdiagnosis and under-diagnosis scenarios. Instrumental swallow assessment like FEES exams is critical, to meet the needs of the dysphagia patient population, by providing precise information regarding the physiology of the pharyngeal phase of the swallow. Given the portability of FEES exams, along with the full color imaging of the pharyngeal phase of the swallow, coupled with the ease to access in settings without dedicated radiology departments for MBS, and the emerging technology with updated equipment, the procedure has shown an increase in use among speech language pathologists.
There are several clinical components that make FEES exams the preferred instrumental assessment, as the exam can directly access surface anatomy changes, secretions management, and patient endurance/stamina as it relates to dysphagia with an uninterrupted ongoing recording. Lastly, with a traditional MBS exam, staff are generally only peripherally involved and not present for the exam, given the exposure to radiation and other variables. When FEES exams are done on the hospital or skilled nursing units, staff and family can be present without radiation exposure, giving them direct involvement in the exam and enhancing the education/interdisciplinary process.
SUE: What are some examples of delays and problems caused by reusable scopes not being available?
Blicker: I have seen firsthand, across many different types of endoscopy brands, the wear and tear that develops with a traditional endoscope with repeated usage. There are variables in cleaning and usage that result in some scopes needing frequent repair. When a reusable endoscope is not working, which can happen, it is not always easy to get a loaner endoscope. This may cause delays to exam access. This is not an issue with single-use scope technology.
SUE: What are some of the key advantages of single-use endoscopes in FEES exams?
Blicker: Portable, lightweight, requires limited space, excellent for family/staff/patient training right at the bedside, no need to transport a reusable scope across the hospital to be cleaned, instant information is available.
SUE: What type of facilities that perform FEES exams would benefit most from single-use scopes?
Blicker: Sub-acute rehabilitation hospitals, skilled nursing facilities, outpatient office settings, long-term acute care hospitals, and acute care hospitals are good candidates for single-use devices. Skilled nursing facilities do not have endoscopy departments to clean their reusable endoscopes, so they must do it on their own. Similarly, in long-term acute care hospitals, where SLPs may be cleaning their own reusable endoscopes, it can be costly and potentially disrupt the flow of the workday. Most skilled nursing facilities do not have dedicated onsite radiology departments, to schedule modified barium swallows. For the dysphagia patients who need testing in these facilities, FEES exams are a great onsite solution.
SUE: How useful is frame-by-frame video replay capability to your clinical practice?
Blicker: It is essential to truly appreciate swallow physiology when reviewing your exam. Video replay allows the clinician access to these critical events.
SUE: The mobile segment has seen growth over the past 10 years. When and where is single-use advantageous to mobile providers?
Blicker: Infection control and high-level disinfection can be challenging for mobile providers who travel to multiple facilities throughout the day while practicing with reusable endoscopes. During these challenging times with COVID-19, single-use endoscopy is an effective option as they do not require high-level disinfection. You essentially remove the high-level disinfection component. Additionally, it is far easier to transport a single-use system.
SUE: What happens to patients when testing cannot be done in an acute setting and they are being discharged?
Blicker: Overdiagnosis and underdiagnosis regarding aspiration risk from clinical exams can take place, which can have negative outcomes. The clinical exam does not allow for objective data to be obtained regarding swallow physiology. This can only be done with instrumental assessment like bedside flexible rhinolaryngology exams or modified barium swallow tests. If your patient doesn’t get their needed test, in acute care, they may have a setback once discharged, in relation to their dysphagia, and have to be readmitted the following week.
SUE: What makes the lightweight structure of disposable devices an advantage for speech language pathologists?
Blicker: The lightweight component of [single-use] scopes makes them very user-friendly for the speech language pathologist and patient, and there is less arm fatigue in longer exams. Our exams go longer than the ENT endoscopic exams since we are feeding the patient. It matters significantly.
SUE: Have you heard of large hospitals where FEES exams were limited to one a day because scopes needed to be picked up by courier and transported miles away to be cleaned? Why is this a problem?
Blicker: I have heard of this, and I have seen this with my own eyes. Some hospital systems actually have couriers that pick up the scope and drive it to another location for high-level disinfection for a reusable scope. It is a problem because it limits patient access to care.
SUE: Do you think many facilities could benefit from a cost analysis of how much they can save by converting to single-use scopes?
Blicker: Yes, sub-acute rehabilitation hospitals, skilled nursing facilities, long-term acute care hospitals, and acute care hospitals. I think many hospitals would benefit from a cost analysis of the money spent on high-level disinfection: endoscopy staff, infrared thermometers, gowns, gloves, goggles, pH test strips, leak tester, containers for storage, the actual high-level disinfectant, time spent disinfecting, storage containers for reusable scope when not in use, basins for use during high-level disinfection, vs. single-use scopes.
SUE: What are the limitations to more people doing FEES exams?
Blicker: Education, training, financial limitations, reimbursement changes, and lack of access to equipment. A limiting factor to more growth in this field is often lack of mentorship.