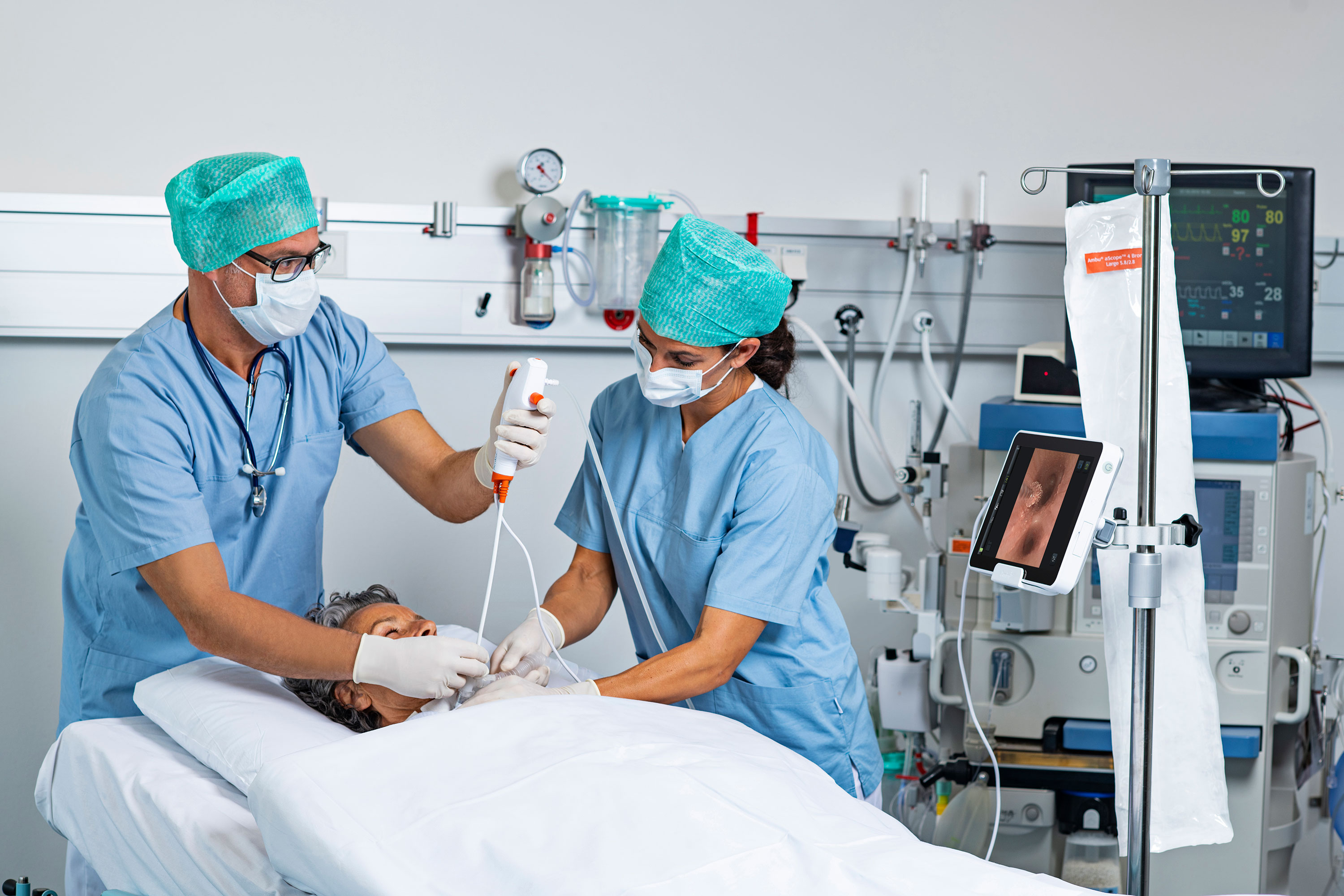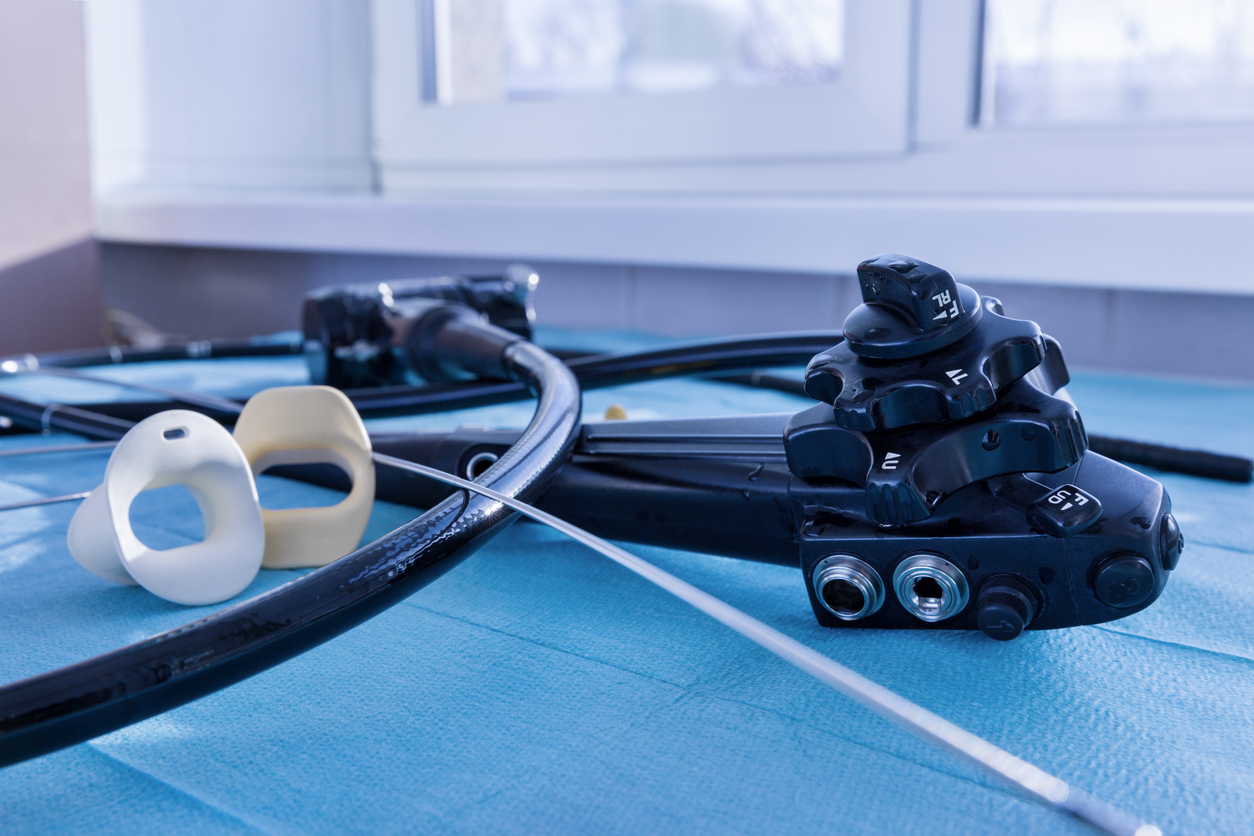
Even without an infection outbreak, duodenoscopes may still be contaminated.
In fact, a recent study including 16 clinical sites across the U.S. detected a 5.3 percent contamination rate of duodenoscopes after reprocessing in non-outbreak settings.
During the study period of October 2018 through September 2019, researchers collected samples from 859 “newer-model” duodenoscopes and 850 “older-model” scopes. Thirty-five of the newer-model duodenoscopes (4.1 percent) harbored high-concern organisms, which were found in 56 older-model (6.6 percent) scopes.
High-concern organisms were of gastrointestinal origin in 45.4 percent of identified cases. Other classifications included non-gastrointestinal human origin (16.7 percent), environmental (24.1), and unidentified (0.9).
The study investigated duodenoscope contamination rates by “viable” microorganisms following manufacturers’ FDA-cleared reprocessing instructions. This means scopes were sampled after bedside cleaning, manual cleaning, and automated reprocessing, including high-level disinfection.
Fifteen of the 16 sites had some high-concern contamination detected. Additionally, a retrospective review found improper reprocessing in 26 of 94 samples and improper sampling 42 of 101 samples.
“If duodenoscopes are properly disinfected, but the environment is contaminated, the scopes may become contaminated after reprocessing during handling without gloves, storage with moisture in channels, and/or during endoscope sampling,” the authors write. “Ensuring dry storage is crucial to preventing biofilm formation in endoscope channels during storage.”
Researchers reviewed reprocessing and sampling techniques when high-concern organisms were detected. In more than 41 percent of those cases, they found that improper handling was caused by inappropriate personal protective equipment or improper aseptic techniques, “which may have caused accidental environmental contamination of reprocessed endoscopes.”
The authors emphasize that infection and contamination are not synonymous. Post-endoscopy infections can be either endogenous or exogenous. Most are endogenous, meaning they arise from patients’ microbiota and are not prevented through reprocessing or sterilization. Exogenous infections come from contaminated endoscopes. The rate of infectious complications following ERCP is between 2 percent and 4 percent and pancreatitis is the most common.
“Attempts should continue to be made to further reduce contamination rates,” the authors conclude. “Additional improvements to the manufacturer’s instructions for use, human factors during the reprocessing procedure, ongoing training programs, cleanliness of reprocessing environments, and the design of the distal end of the duodenoscope should be considered.”
The FDA recently updated a safety communication in which it calls for a transition to duodenoscopes with innovative designs “that make reprocessing easier, more effective, or unnecessary.”